Double Threat
The impact of climate change on human health
April/May 2018Statements of fact and opinions expressed herein are those of the individual author(s) and are not necessarily those of the Society of Actuaries or the respective authors’ employers.
Climate influences much of the world around us, and many aspects of climate are taken for granted. The seasons, crops growing, flowers blooming, insects emerging—these are just some examples of what climate controls.
The medical field has long understood that climate can regulate human health. Hippocrates, the ancient Greek physician who is one of the leading historical figures in medicine, documented abnormal changes in local weather in his reports describing disease outbreaks.1 In 1814, James Tilton, M.D., then-surgeon general of the U.S. Army, required all military surgeons to record the daily temperature and precipitation records at military hospitals, because he understood that changes in weather were directly tied to the health of soldiers.2 Those early weather observations recorded by the army surgeons now comprise some of the first climate records for the United States.
In present-day medicine, there are both anecdotal stories and extensive scientific evidence describing the links between changes in climate and the occurrence of diseases, deaths, injuries and various other health outcomes. Thus, if our climate changes, we can expect that health outcomes will also change.
Climate Change and Health
In 2016, the White House released a report detailing the impacts of climate change on human health.3 One of the key findings of that report was that “climate change is a significant threat to the health of the American people.” This statement seems bold, considering all of the different health threats we face on a regular basis. You might start asking:
- “How is climate change linked to my health?”
- “Why would warmer temperatures bother me?”
The links between climate and health are not always apparent to the casual observer, but the connections are there. Changing one component in our climate, such as the global temperatures, can also cause other aspects of the environment around us to change (including increases in air pollution, changes in disease prevalence, exposure to deadly heat waves and numerous other effects; see Figure 1). Thus, we should expect that changing the thermostat of the Earth would have additional consequences on our health.
Figure 1: Potential Link Between Climate and Health Outcomes
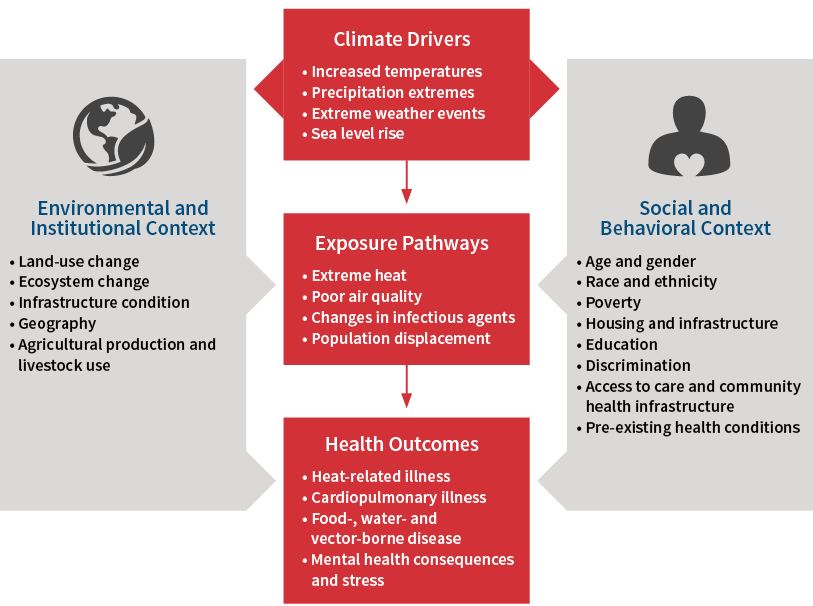
Source: Crimmins, Allison, John Balbus, Janet L. Gamble, Charles B. Beard, Jesse E. Bell, Daniel Dodgen, Rebecca J. Eisen, Neal Fann, Michelle D. Hawkins, Stephanie C. Herring, Lesley Jantarasami, David M. Mills, Shubhayu Saha, Marcus C. Sarofim, Juli Trtanj, and Lewis Ziska, (eds.). 2016. The Impacts of Climate Change on Human Health in the United States: A Scientific Assessment. Washington, D.C.: U.S. Global Change Research Program. http://dx.doi.org/10.7930/J0R49NQX.
As many of us live in industrialized nations with limited exposure to the elements, we can typically minimize the effects of weather and climate on our daily lives. We do that by living indoors, wearing weather-appropriate clothing or limiting our time in conditions that we find uncomfortable. These minor adjustments do not mean that climate change will not affect our health—it simply means that those with the resources to adapt to climate change are less likely to experience as many negative outcomes as those with fewer resources.
Changes in Extreme Events Lead to Health Outcomes
Changes in extreme events lead to some of the most easily seen and understood health impacts from climate change. In 2017, the United States experienced grim reminders of the human and economic costs of these extreme events, which included 16 disasters that in total exceeded $300 billion in cost and resulted in more than 360 attributed deaths. Evidence consistently has shown that some extreme events (such as heat waves, droughts and flooding rains) are becoming more intense and frequent. (See “Observing Mother Nature” for more information.)
Each year, extreme weather and climate events are directly responsible for thousands of deaths and injuries around the world. The natural line of reasoning would allow you to conclude that as these events get stronger, the potential ramifications will only become greater. Research is starting to explore this link, and early results have shown that more deaths are occurring as a result of some of these extreme events being more intense and frequent because of human-caused climate change.4 Because these increases in severity and frequency are projected to continue in the future, the corresponding number of deaths and injuries could also increase.5
Pathogens and Climate Change
The changes in climate that we have experienced during the last century—and will face in the coming century—change other aspects that influence our health. Climate plays a critical role in biological activity. By this, I mean where and when things can live. As temperatures rise and precipitation patterns change, the climate begins to become more hospitable for some organisms and less favorable for others.
Over the past century, there are reports of disease-carrying mosquitoes moving north into new habitats as temperatures warm and precipitation patterns change. Studies also have shown a link between higher temperatures and the spread of the North American tick, Ixodes scapularis, that carries Lyme disease.6 As ocean temperatures have increased over the last century, Vibrio infections—from a pathogenic bacterium that lives in coastal waters—are now occurring at higher latitudes.7 The infections from this bacteria can come from eating contaminated oysters or from exposed wounds, with effects ranging from mild gastrointestinal illness to severe infections and even death. These are just a few of the many examples of climate change contributing to the spread of infectious diseases.
As climate continues to change, new disease threats may emerge. It is difficult to say exactly what will be next, because diseases are constantly evolving and developing. A few years ago, little attention was given to the Zika virus, an often overlooked disease spread by mosquitoes. This virus is now a major concern of many public health officials across the globe. Although it is difficult to determine what, if any, link there is between the recent outbreak of Zika virus to climate change, the future increases in temperature and changes in precipitation could help spread this disease and other similar ones.
Respiratory Illness and Climate Change
Other alterations to our environment from climate change can lead to serious health consequences. As carbon dioxide increases in the atmosphere and the growing season lengthens due to the resulting rise in temperature, some of the plant life around us is thriving and doing quite well. At first, this seems like a positive effect of climate change, which is partly true. However, as plants thrive, some release pollen in the air for reproduction. The more the plant thrives, the more pollen it produces. For those of us who suffer from allergies, this release of pollen can be very burdensome and can create unpleasant allergic reactions to going outside. For those 300 million people worldwide who suffer from asthma or other serious respiratory issues, pollen in the air can be a serious threat to life. Ragweed, a common plant that produces highly allergenic pollen, has experienced an increase in the length of its pollen season by 13 days to 27 days due to increases in temperature over the last couple of decades.8
The lengthening of the growing season and increased production of vegetation can have another consequence. Wildland fires have been starting earlier in the year and are lasting longer. This is partly due to the management practices that have suppressed wildland fires, which can cause them to erupt into very intense fires, but our changing climate is also to blame, as temperatures are increasing and droughts are becoming more common.9 Not only do these fires cause destruction of property and deaths associated with the fire, the smoke can travel hundreds of miles and cause respiratory ailments for anyone in the path.
Mental Health and Climate Change
For those who face the aftermath of a natural disaster, such as a hurricane, severe drought or wildfire, the health consequences may not always be apparent. Loss of loved ones, property, employment and displacement from homes can have long-lasting effects on individuals or communities that live through these events. People who experience these climate-related events can suffer from post-traumatic stress disorder, increased anxiety and depression, which can lead to long-term mental health issues.
Climate change can also lead to the displacement or migration of people seeking to escape the environmental threats they previously faced. For example, this can happen when an extreme event forces individuals to suddenly move to new locations to escape the destruction of a storm. Gradual change can also cause the environment around a community to become inhospitable. Some island nations of the Pacific Ocean are already looking for new places to live as rising sea levels slowly make their islands uninhabitable. Not only are the oceans overtaking their lands, but the freshwater on their islands is no longer potable because of the salt water intrusion. People in these circumstances can lose their cultural identity as they try to adjust to new ways of life.
Conflict and Climate Change
As populations are forced to relocate, communities and systems of government will need to accommodate these people. These groups may temporarily occupy a new location, as with the mass migration of people seeking reprieve from the devastation of an extreme event, or they may relocate permanently, as with populations whose previous homes can no longer sustain their existence. Assisting these populations during and after their displacement can be costly, because they will need support and assistance to establish themselves in their new homes.
Unfortunately, mass migration can lead to conflict and turmoil if residents of the host location are opposed or resistant to the influx of newcomers. Combining two distinct groups of people can lead to conflict. Strife can also arise if a particular population is unable to adapt or deal with the environmental pressures faced because of climate change. Some debated evidence suggests that the conflict unfolding in Syria may have been sparked by climate change.10 The drought that preceded, and potentially contributed to, the Syrian conflict was shown to be intensified by climate change.
Although some debate exists on the relationship of this drought to the conflict that followed, the basic model of a severe climate-related event leading to something similar to the Syrian conflict easily can be imagined. First, a climate-related event causes a group of people to experience severe distress. If that group is then unable to find the resources needed to adequately sustain their livelihoods, they may become frustrated and hostile toward the systems of government or groups that they believe responsible for their difficulties. Depending on the manifestation of this situation with the various parties involved, fighting and conflict can be one of the potential outcomes. However, a number of other factors are needed to cause this chain of events to unfold, but the potential for climate change to cause or exacerbate civil unrest is possible given certain conditions.
How Will Populations Cope?
Are all populations vulnerable to the health impacts associated with climate change? Yes. However, some populations are more vulnerable to climate change than others. People who typically are more vulnerable are the very old, the very young, those with fewer financial or societal resources, workers in certain occupations and individuals with preexisting medical conditions. (See “The Vulnerable” by Sam Gutterman for more information.)
Because of the number of people who are vulnerable to these threats, public health agencies throughout the world are starting to take notice of climate change as a health threat. Officials who work for these agencies are creating plans that will help communities prepare for the health effects associated with climate change. Empowered with the best scientific information available, local communities can reduce the risks associated with changes in diseases, injuries and deaths that will come from climate change. Some of these health agencies are accomplishing this work with external funds, but many institutions are devising plans without much support. This work has an added benefit for these communities, as the plans created by public health agencies to address climate change also prepares communities for many other potential disasters and associated risks.
The goal of this article is to illustrate that climate change poses a threat to our health, and to bring awareness to these issues. Although many topics discussed here are concerning, there is still an opportunity for our communities to address these health issues caused by climate change before they become more problematic.
- We can invest in clean technologies, such as renewable energy sources and energy efficient products, that reduce the production of greenhouse gases that cause anthropogenic climate change.
- We can improve existing infrastructure or create new infrastructure to reduce the potential consequences of climate change. Improvements of infrastructure near coastal regions are especially important, as these areas are generally more susceptible to the effects of climate change than other regions, with the continued rising of sea levels along with more frequent flooding and increasing population density.
- We can work across sectors and institutions to understand potential threats and develop new strategies to combat these issues. Public health agencies should not be the only institutions trying to address the negative health outcomes associated with climate change. Mitigation and preparation can start with a variety of private and public institutions, including hospitals, health care providers, sanitation services and utility companies.
- We can expand our research efforts to identify the future health risks associated with climate change in order to take a more proactive approach to health care. Because climate change is already occurring, research could help determine the current excess burden and costs on health care.
By working to address the issues identified in this article, communities have an opportunity to reduce their vulnerability to the health impacts of climate change while improving public health, safety and well-being, and reducing potential costs at the same time.
References:
- 1. Hippocrates, G.E.R. Lloyd, John Chadwick, and William Neville Mann. 1978. “Airs, Waters and Places.” Essay. In Hippocratic Writings. London: Penguin. ↩
- 2. Brown, Harvey E. 1873. The Medical Department of the Unites States Army From 1775 to 1873. Surgeon General Office, Washington, D.C. ↩
- 3. Crimmins, Allison, John Balbus, Janet L. Gamble, Charles B. Beard, Jesse E. Bell, Daniel Dodgen, Rebecca J. Eisen, Neal Fann, Michelle D. Hawkins, Stephanie C. Herring, Lesley Jantarasami, David M. Mills, Shubhayu Saha, Marcus C. Sarofim, Juli Trtanj, and Lewis Ziska, (eds.). 2016. The Impacts of Climate Change on Human Health in the United States: A Scientific Assessment. Washington, D.C.: U.S. Global Change Research Program. http://dx.doi.org/10.7930/J0R49NQX. ↩
- 4. Mitchell, Daniel, Clare Heaviside, Sotiris Vardoulakis, Chris Huntingford, Giacomo Masato, Benoit P. Guillod, Peter Frumhoff, Andy Bowery, David Wallom, and Myles Allen. 2016. “Attributing Human Mortality During Extreme Heat Waves to Anthropogenic Climate Change.” Environmental Research Letters 11 (7) doi:10.1088/1748-9326/11/7/074006.. ↩
- 5. Mora, Camilo, Bénédicte Dousset, Iain R. Caldwell, Farrah E. Powell, Rollan C. Geronimo, Coral R. Bielecki, Chelsie W. W. Counsell, Bonnie S. Dietrich, Emily T. Johnston, Leo V. Louis, and Mathhew P. Lucas. 2017. “Global Risk of Deadly Heat.” June 19. Nature Climate Change. ↩
- 6. Ogden, Nicholas H., Milka Radojevic, Xiaotian Wu, Venkata R. Duvvuri, Patrick A. Leighton, and Jianhong Wu. 2014. “Estimated Effects of Projected Climate Change on the Basic Reproductive Number of the Lyme Disease Vector Ixodes Scapularis.” Environmental Health Perspectives 122 (6): 631–638. ↩
- 7. Baker-Austin, Craig, Joaquin A. Trinanes, Nick G. H. Taylor, Rachel Hartnell, Anja Siitonen, and Jamie Martinez-Urtaza. 2013. “Emerging Vibrio Risk at High Latitudes in Response to Ocean Warming.” Nature Climate Change 3 (1): 73–77. ↩
- 8. Ziska, Lewis, Kim Knowlton, Christine Rogers, Dan Dalan, Nicole Tierney, Mary Ann Elder, Warren Filley, Jeanne Shropshire, Linda B. Ford, Curtis Hedberg, and Pamela Fleetwood. 2011. “Recent Warming by Latitude Associated With Increased Length of Ragweed Pollen Season in Central North America.” Proceedings of the National Academy of Sciences 108 (10): 4248–4251. ↩
- 9. Westerling, A.L., H.G. Hidalgo, D.R. Cayan, and T.W. Swetnam. 2006. “Warming and Earlier Spring Increase Western U.S. Forest Wildfire Activity.” Science 313 (5789): 940–943. ↩
- 10. Kelley, Collin P., Shahrzad Mohtadi, Mark A. Cane, Richard Seager, and Yochanan Kushnir. 2015. “Climate Change in the Fertile Crescent and Implications of the Recent Syrian Drought.” Proceedings of the National Academy of Sciences 112 (11): 3241–3246. ↩


 As climate continues to change, new disease threats may emerge. It is difficult to say exactly what will be next, because diseases are constantly evolving and developing.
As climate continues to change, new disease threats may emerge. It is difficult to say exactly what will be next, because diseases are constantly evolving and developing.