Can We Achieve More for Less?
The impact of technology on health care
November 2020Photo: iStock.com/metamorworks
Defining Innovation
Innovation is any combination of activities or technologies that break existing performance tradeoffs in the attainment of an outcome, in a manner that expands the realm of the possible.
Innovation in health care is defined as providing “more for less”—more value, better outcomes, greater convenience, access and simplicity; all for less cost, complexity and time required by the patient and the provider, in a way that expands what is currently possible.1
Reference:
1. Deloitte. 2016. Top 10 Health Care Innovations: Achieving More for Less. Deloitte Center for Health Solutions.
Today, technology is synonymous with speed and convenience. As technology has improved, our expectations as consumers have grown accordingly. The average click-to-door speed of an Amazon order almost halved from 2015 to 2018.1 By the standards of consumer convenience, technology has allowed us to expand the art of the possible with the click of a button.
When considering how portable these efficiencies are to an area as essential as health care, the central question is: How can more value and impact be delivered for less cost? This is not a matter of delivering the latest health gadget to a savvy audience; rather, we are searching for how to improve modern health and the health care ecosystem by leveraging the efficiencies technology affords.
Research from McKinsey notes that people naturally prioritize robust health care coverage when assessing insurers. However, this is followed by customer service, access and cost. When it comes to customer service and access, people have very specific mental models in mind: When asked what health care companies should model themselves after, people often cite innovative technology companies like Google, Apple and Amazon, which are all champions of the “more for less” modality.2
The COVID-19 pandemic has accelerated this urgency toward a digital experience in health care. Individuals need remote access to their health care network; they are empowered by having access to their health data; they seek the convenience of ordering refill medications from the safety of their homes. In short, consumers are demanding a frictionless process that health technology can now afford them, as has been done in other spaces.
Yet, while 70 percent of people prefer digital health care solutions, only 49 percent of them use the technologies their health insurers provide. And when they do use this technology, it is not necessarily for value-added services like telehealth, but to perform the most basic of functions: updating their personal information.3
This means that successful providers will need to master the digital realm by creating tools that consumers can access easily, engage with, and in which they can find true utility. People want to engage in their care to improve their health outcomes and minimize cost, but it starts by having access to personalized and relevant content that will help educate and steer them toward successful outcomes in an expedient manner.
Investments can and should be made in artificial intelligence (AI) and other technologies that optimize engagement and operational efficiencies. But if health care providers do not meet the consumer at their unique starting point and become an evolving ally and assistant along their health care journey, the gains will be diminished unnecessarily. If, however, that important connection is brokered, a win-win situation may be created for consumers and providers.
Health Technology Empowers Individuals by Facilitating a “More for Less” Modality
To achieve more for less, we must understand why there is a disjuncture between the perceived value of technology and health care costs. This is due in part to the fact that novel technologies have been shown to be insufficient at driving down health care costs and, in some instances, directly contribute to the increase in expenditure. Health care economists estimate 40 percent to 50 percent of annual cost increases can be traced to new technologies or the intensified use of old ones, which makes the control of technology the most important factor in bringing down health care costs.4
Innovation in and of itself does not guarantee productivity and efficiency, and thus, when the result of innovation is low productivity, health care costs continue to climb. Low-productivity innovation tends to be content-based as opposed to processed-based, performance-enhancing rather than cost-reducing, additive to patient care rather than substitutive to patient care and business-model sustaining rather than disrupting. Low-productivity innovation should be replaced with technology that improves processes, creates a system of cohesion and ultimately lowers costs while replacing traditional procedures.5
Products like wearables are not simply another gadget, but rather they are mechanisms with which patients become empowered through the ability to be a part of their health care experience, facilitated by the instant connection to electronic health records (EHRs), real-time health data and seamless data sharing with their health care provider teams. AI is being used to streamline the patient experience, helping health care facilities better manage patient flow and data processing.6 Telehealth is disrupting the business of health care, providing increased access to services, continuity of care and improved remote patient monitoring (RPM) for chronic care conditions.7 These high-productivity innovations should be the focus of future innovations in health care when trying to achieve more for less.
The successful implementation of a high-productivity system of innovations can impact health care on three levels:
- Improved care delivery models through seamless data and information exchange
- The power of data harnessed through advanced analytics and transparency
- Process automation
Digital solutions like telehealth can improve the efficiency of monitoring patients at home, thereby avoiding costly hospital stays, and EHRs can help ensure adherence to appropriate clinical practice. Health care data analytics, machine learning and algorithms create decision-support tools and other online services to help providers make the best clinical decisions around diagnosis and treatment. Process automation also helps to increase efficiency in health care settings through the digitization of appointments, patient records and hospital billing.8
Optimizing the digital value chain is a worthwhile investment because the innovations in the space are laden with so much potential—from telehealth to AI, as summarized in a sampling of case studies in Figure 1. What is needed then is a governance system that ensures consumer health technology serves high-productivity innovation by maximizing process improvement while minimizing cost across the health care ecosystem.
Figure 1: Examples of Achieving “More For Less” Through Different Digital Applications
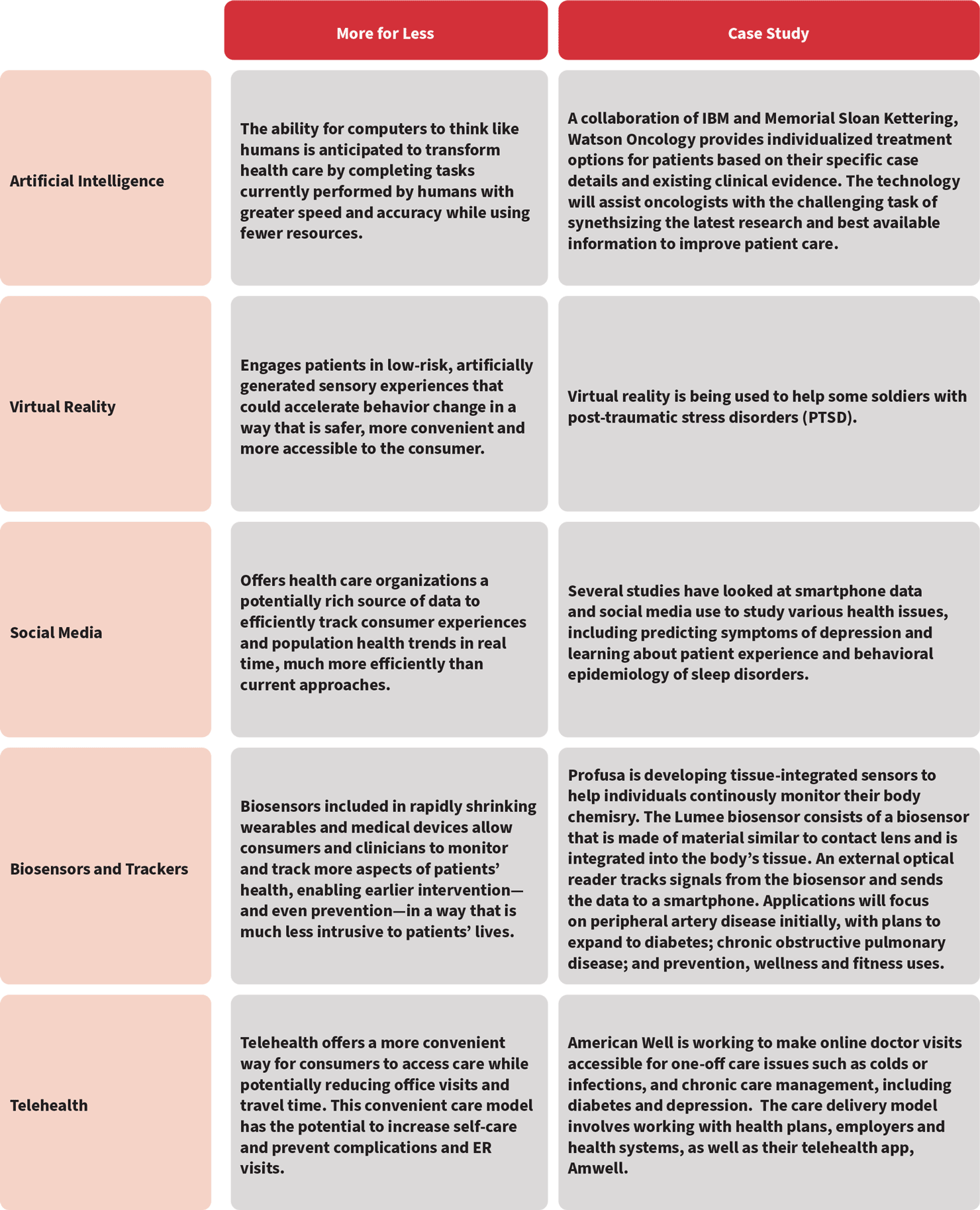
Source: Deloitte. 2016. Top 10 Health Care Innovations: Achieving More for Less. Deloitte Center for Health Solutions.
Delivering on the Promises of “More for Less”
While 2020 has forced us to rethink how we envision the future of health, it is also a time to reflect on how far we have come and whether we have delivered on some of the promises envisioned for 2020.9
Wearables Are More Prevalent, but More Impactful and Scalable Condition-Management Tools Powered by Data and Design Are Required
Activity-tracking wearables have become increasingly prevalent. With step counters now a standard feature on most mobile phones, more people have a greater awareness of their activity levels, which is an important starting point for behavior change.
While condition-management devices have advanced by a considerable degree, only gradual progress has been made on broadening their domain of application. Diabetes management is one area that has seen a transformation over the past few years, whether in the form of continuous blood sugar monitoring or, more recently, in closed-loop systems that actively monitor blood sugar levels and adjust insulin levels automatically.10
Importantly, effective devices are not solely a function of technology—central to the success of consumer health technology is the merger of digital, data and design. One such example, Ascencia—in partnership with IDEO, a world-renowned design company—has turned to a modern technology design modality to help remove the stigma of checking blood sugar levels. They create a user experience in which individuals are provided with contextual messages about their glucose readings relative to their personalized goals, all framed within the context of their broader lifestyle. This then transforms glucose monitoring from pure information gathering to a personalized and contextualized goal framework for individuals, engaging them in their own health care.11
Integrated Experiences Facilitated Through the Internet of Medical Things Are Needed to Drive Awareness and Appropriate Use
Devices and their data have a very particular application: empowering the individual to be an active participant in their own health care by forging a meaningful partnership with their provider. This is an area that we are edging toward with EHRs and fast health care interoperability resources (FHIRs), bridging the gap between health records, standard application programming interfaces (APIs) and devices so information can be exchanged seamlessly. Unfortunately, this remains a nascent area, and while data sharing is the first step, empowering the user in their self-management with meaningful and actionable data will require careful deliberation. Effective data parity is the gold standard to which we aspire—until knowledge-sharing is honed, it will be an ongoing struggle to improve awareness, self-management and prevention that is so critical to the health care space.
Internet of Medical Things
The Internet of Medical Things is a connected infrastructure of medical devices, software applications, and health systems and services.1 The Internet of Medical Things market consists of smart devices, such as wearables and medical monitors, strictly for health care use on the body, in the home, or in community, clinic or hospital settings; and associated real-time location, telehealth and other services.2
References:
1. Steger, Andrew. How the Internet of Medical Things Is Impacting Healthcare. Health Tech Magazine, January 16, 2020.
2. Alliance of Advanced BioMedical Engineering. 2017. Internet of Medical Things Revolutionizing Healthcare. The American Society of Mechanical Engineers.
To truly harness the power of technology requires cohesion. When we think about what makes internet companies so proficient, it is their ability to embed assets in an experience that comes together intuitively for the user. In a similar manner, we need ecosystems like the Internet of Medical Things (see sidebar) that draw assets together for the consumer to manage their health holistically.
The benefits of such a system are clear: At the center of this model, we have improved patient outcomes that necessitate an enhanced patient experience, remote monitoring of chronic diseases, improved disease management, improved diagnosis and treatment, decreased costs and improved drug management. In short, if the Internet of Medical Things delivers on its promise, there will be a wealth of value for patients, providers and payors.12
Accessibility Needs to Be Solved From a Cost and Design Perspective
As with all consumer technology, companies have released more affordable options for health technology over time, but oftentimes large portions of the population for whom the devices remain a non-essential luxury are excluded. Ryan Shaw, a professor at Duke University, notes that “the people who can benefit the most … often have troubles with the usability and utility of many personalized health technologies.”13 Interventions are most effective when they are adopted at scale, with cost serving as a material barrier to adoption. Programs need to be able to better engage underserved communities, including but not limited to older adults and those who are less able to afford this often-valuable technology in the first place.14
Individuals Should be Actively Engaged and Rewarded for Healthy Behavior Change
The question of access is essential because, when given the choice, an overwhelming majority of individuals is willing to change their behaviors to reduce health costs. In a McKinsey study, individuals would happily take 5,000 steps a day per month to get a $10 premium reduction, or meet with a dietician to get a $20 premium reduction.15 This proclivity toward prevention is telling: It speaks to how people are driven to improve their health and reduce their own costs, which would be a victory for insurers and society more broadly that would benefit from healthier individuals.
Incentives are so important because behavioral science teaches us that, while most of us have the best of intentions, we suffer from inertia, present bias and over-optimism bias. However, while behavioral science points to our cognitive errors, it also points to potential solutions. A study published by RAND Europe in 2018 looked at an incentive program for physical activity implemented at Vitality in the United States, the United Kingdom and South Africa. Members opting into the benefit pay a nominal activation fee of $25 for an Apple Watch and sign a two-year contract during which they can earn their Apple Watch for free if they meet their monthly activity targets. While this appears relatively simple, the program combines technology, behavioral science and design to drive healthy behavior change with compelling results. The program not only led to 34 percent increases in activity, but this activity was sustained in individuals across various risk classes.16
Technology Needs to be Funded by a Mix of Employers, Insurers and Providers
In aligning the value chain created by health technology, the hope is that Moore’s Law might be realized in the health space. Moore’s Law refers to when Gordon E. Moore, the co-founder of Intel, forecasted in 1965 that the number of transistors on a microchip would double every two years while the cost of computers would be halved. Applied more generally, Moore’s Law implies that technology will become more efficient and less costly over time. To date, Moore’s Law, when applied to health care, has failed—every 13 years, spending on U.S. health care doubles.17 This is due in part to the fact that the funding systems, both private and public, offer little incentive to use cost-effective medicine, instead paying for treatment that causes no harm regardless of its efficacy.18 Another major contributor concerns the large amounts of funding dollars spent on researching highly specialized drugs and procedures that are advancing the health care of tomorrow, rather than making current health care more efficient.19 To remedy this, the investment in health technology needs to be more disciplined, focusing the spend on treatments that drive material health benefits and savings. Robust clinical and cost evaluations are needed so efficiency can be achieved across the spectrum of health technology—not simply at the leading edge.
One additional aspect of this complicated problem is the gulf between health and health care. While consumers turn to health technology to become healthier, employers and insurers view consumer health technology as a mechanism with which to lower health care costs.20 Currently, employers and insurance companies typically fund health care, with a focus on treatment, while consumers must fund prevention-focused health technologies.
If health technology achieves its ambition—creating healthier individuals and more streamlined health knowledge transfer between individuals and their providers—employers and health insurers have a vested interest in subsidizing this technology.
Protecting Consumers
Governance of AI
AI is pivotal in creating efficiencies and maximizing the potential of the health care system. People today are quite comfortable turning to intelligent technologies like virtual coaches or clinicians that provide them with care from the convenience of their homes. But there are limitations: While individuals are happy to rely on AI to help them book their next appointment or coach them through a nutrition plan, fewer individuals are quite as receptive to meeting a robot in the operating theater.21
AI is championed precisely because chatbots are available when people need them—without spending hours in a doctor’s waiting room. In short, AI stands to make life more convenient.
However, when it comes to the pitfalls of AI—or at least the perceived pitfalls—a strong recurring theme is that individuals do not understand these sophisticated black-box solutions and are skeptical of sharing their most valuable health data to be run through these opaque algorithms.22
Additionally: “AI is making its way into clinical practice. Because of its reliance on historical data, which are based on biased data generation or clinical practices, AI can create or perpetuate biases that may worsen patient outcomes. However, by strategically deploying AI and carefully selecting underlying data, algorithm developers can mitigate AI bias. Addressing bias could allow AI to reach its fullest potential by helping to improve diagnosis and prediction while protecting patients.”23
Earning trust involves stringent governance standards of the use of AI and oversight from expert professionals like actuaries. While there are clear problems with AI, there are natural solutions, and we need to be mindful of the domain experts with whom we collaborate, the questions we ask of the data and the diversity of our underlying data sets.24 It is only by holding ourselves to these high standards that a secure and trusted data-driven ecosystem may be created.
Governance of Data Use
At the heart of the data question is not only how we may create efficiencies in health care, but how we create value for the member. In the United States, the possibility of getting medical records through smartphone apps as easily as you order takeout has brought concerns about privacy. The American Medical Association and others are concerned that unregulated technology companies could sell data or expose sensitive medical information. Proponents, on the other hand, argue that data is an empowerment tool—access to medical data would help individuals better manage their health, solicit second opinions and understand their medical costs.25 This is all moving care to a consumer service model, so people can shop for doctors and insurers on their smartphones as easily as they pay bills or purchase their latest gadgets.
The tension between removing paternalism from the health care system by giving members the freedom to shop for their health care, and the skepticism of relying on technology companies to govern themselves, necessitate external governance.
In 2016, the Vitality Institute developed its guidelines for personalized health technology.26 The question was motivated by reconciling the promise of data—understanding health, modifying behaviors, precision medicine, population modeling—with the pitfalls of data concerns. This was in response to many familiar questions, including:
- Who has access to your data?
- Is your data accurate and reliable?
- Is your data shared or sold?
- How is your data protected from cybercriminals?
The Vitality Institute guidelines touch upon five critical pillars:
- Build health technologies informed by science and be open and transparent about the personal health information you collect and why.
- Scale affordable health technologies by brokering partnerships between the public and private sector and developing innovative financing models that enable win-win situations for individuals, companies and governments.
- Guide the interpretation of health data and make it easy for consumers to access and control the sharing of their personal health information and empower them to do so. To this end, diverse individuals—linguistically, culturally and from a health literacy perspective—should be involved in the testing process, and we should be cognizant of the way we share data with individuals and how different people value and understand this important data.
- Protect and secure health data.
- And, finally, we must govern the responsible use of health technology and data by being accountable for practices and promises. This means that corporate boards and senior management should embrace and articulate publicly the values of responsibly innovating for corporate and societal benefits.
Sharing in the Value Created by Health Technology
An era of consumerism that engages and empowers consumers in their own health decisions is having profound implications for the prevention and management of complex and costly diseases. Personalized health technologies that enable consumers to track their health remotely can support physicians in delivering precision medicine and help academics uncover variations in health behaviors among disparate populations.
If the COVID-19 pandemic has taught us anything, it is that we need to be continuously preparing for the next crisis— establishing the frameworks for systematic efficiencies and better health outcomes as a function of digital health, data, design and scientific oversight. As a profession, actuaries are well-positioned to study and opine on how to govern and optimize the funding of health technology. Success in this regard will also entail reframing our thinking on technology as a linchpin within a shared-value ecosystem—one in which technology is the enabler of different parties working toward a shared goal (healthier individuals) and sharing in the value created for all.
References:
- 1. Rakuten Intelligence. Marriott Tries Home Sharing, Amazon Ups the Ante on Shipping Speeds.” Rakuten Intelligence, May 6, 2019. ↩
- 2. McKinsey & Company. 2018. Healthcare Consumerism 2018: An Update on the Journey. ↩
- 3. Ibid. ↩
- 4. Callahan, Daniel. 2008. “Health Care Costs and Medical technology.” In From Birth to Death and Bench to Clinic: The Hastings Center Bioethics Briefing Book for Journalists, Policymakers, and Campaigns, 79–82. Garrison, New York: The Hastings Center. ↩
- 5. Cahan, Eli M., Robert Kocher, and Roger Bohn. Why Isn’t Innovation Helping Reduce Health Care Costs? Health Affairs, June 4, 2020. ↩
- 6. Daley, Sam. Surgical Robots, New Medicines and Better Care: 32 Examples of AI in Healthcare. BuiltIn, March 25, 2020. ↩
- 7. Gorke, Jeff. Telehealth Continues to Change the Face of Healthcare Delivery—For The Better. Forbes, September 24, 2019. ↩
- 8. London, Thomas, and Penelope Dash. Health Systems: Improving and Sustaining Quality Through Digital Transformation. McKinsey, 2016. ↩
- 9. Deloitte. 2014. Healthcare and Life Sciences Predictions 2020: A Bold Future? Deloitte Centre for Health Solutions. ↩
- 10. Allen, Natalie, and Anshu Gupta. 2019. Current Diabetes Technology: Striving for the Artificial Pancreas. Diagnostics 9, no. 31. ↩
- 11. IDEO. 2019. A Holistic, Human-Centered Approach to Managing Diabetes Care. ↩
- 12. Deloitte. 2019. 2019 Global Health Care Outlook: Shaping The Future. ↩
- 13. Vitality Institute. 2016. Guidelines for Personalized Health Technology: Final Report. ↩
- 14. Patel, M. S., L. Foschini, G. W. Kurtzman, J. Zhu, W. Wang, and C.A. Rareshide. 2017. Using Wearable Devices and Smartphones to Track Physical Activity: Initial Activation, Sustained Use, and Step Counts Across Sociodemographic Characteristics in a National Sample. Annals of Internal Medicine 167:755–757. ↩
- 15. Supra note 2. ↩
- 16. Hafner, Marco, Jack Pollard, and Christian Van Stolk. 2018. Incentives and Physical Activity: An Assessment of the Association Between Vitality’s Active Rewards With Apple Watch Benefit and Sustained Physical Activity Improvements. Santa Monica, California: RAND Corporation. ↩
- 17. Regalado, Antonio. We Need a Moore’s Law for Medicine. MIT Technology Review, September 3, 2013. ↩
- 18. Pew Research Center. 2019. About One-in-Five Americans Use a Smart Watch or Fitness Tracker. ↩
- 19. Skinner, J. S. The Costly Paradox of Health-Care Technology. MIT Technology Review, September 5, 2013. ↩
- 20. Interdisciplinary Center for Healthy Workplaces. 2015. Health Technology in the Workplace: Leveraging Technology to Protect and Improve Worker Health. University of California – Berkeley. ↩
- 21. Accenture. 2018. Accenture 2018 Consumer Survey on Digital Health. ↩
- 22. Ibid. ↩
- 23. Parikh, Ravi B., Stephanie Teeple, and Amol S. Navathe. 2019. Addressing Bias in Artificial Intelligence in Health Care. JAMA 322, no. 24:2,377–2,378. ↩
- 24. Gianfrancesco, Milena A., Suzanne Tamang, Jinoos Yazdany, and Gabriela Schmajuk. 2018. Potential Biases in Machine Learning Algorithms Using Electronic Health Record Data. JAMA Internal Medicine 178, no. 11:1,544–1,547. ↩
- 25. Supra note 23. ↩
- 26. Supra note 13. ↩
Copyright © 2020 by the Society of Actuaries, Chicago, Illinois.

